The First 3 Days
** Very Useful information for First Timer Mother **
<Support Us via "Like" our facebok Page and Share>
Scene 1: The Hospital. You have just delivered a beautiful, perfect baby. He sleeps like an angel in the nursery, in your room. You gloat to all friends and family about your wonderful feeder and sleeper. A few days later, you are discharged and take him home.
Scene 2: Home, Day 3. The honeymoon is over...Your baby is feeding frequently and for long periods of time. His sleep patterns have miraculously changed and he is awake all night, crying more often. You feel, "What have I done wrong? He was so perfect in the hospital!" The answer is: Absolutely nothing! This is, fortunately or unfortunately, normal.
What to Generally Expect at This Stage
Whether a baby is exhausted from the long journey into this world, sleeping heavily because of the hum of activity in the nursery or because he is being held against your warm body, babies generally sleep well in the hospital. (Moms who have had C-sections are often more realistic in their expectations once they go home because they are in the hospital a bit longer, which means that their babies "wake up" while they're in the hospital.) Once they come home, everything changes: Feedings are much more frequent and last longer and sleep patterns adjust because of the new schedule. Some babies feed for what may seem like hours and then sleep for many hours. Once the milk comes in, patterns change yet again!
Common Issues For Mother at This Stage
Aside from physical exhaustion kicking in, sore nipples continue to be the most common issue in the first three days postpartum. At this stage, even with a properly latched baby, nipple sensitivity is still prevalent because of postpartum hormonal changes. However, if nipples are cracked, bleeding, or blistering, the latch-on needs help. Contact a lactation consultant immediately.
Some moms also find that their milk has started to transition from colostrum to transitional milk by Day 3. They often feel a heaviness to their breasts, which indicates that their milk is starting to "come in." Feeding frequently will combat any discomfort.
Common Issues For Baby at This Stage
Jaundice is common in breastfed babies. However, by breastfeeding frequently (at least 8 to 10 times a day) in the first 3 days of life, you can greatly reduce the chances that your baby will require higher intervention, such as phototherapy (going under bilirubin lights.)
Sleepiness may also prevail...
Waking Up A Sleepy Baby
Your body is in the process of building a milk supply that will fully sustain your baby and your baby needs frequent feedings for her growth and development. It is essential for both the establishment of your milk supply and the baby's nutrition to continue to wake the baby if he is not waking himself. Some people or books may tell you that you should never wake a sleeping baby. While that may be true later -- after your milk supply is established and the baby is showing all signs of feeding well -- at this stage it is very important.
Establishing A Milk Supply
At this stage, you will notice your breasts becoming fuller and heavier. Your milk is "coming in!" Your milk is changing from colostrum to transitional milk and you will notice the color changing from a clear, yellowish fluid (colostrum) to a thicker white (transitional milk). Continue to breastfeed (or, if necessary, pump) every 2 to 3 hours to stimulate supply.
If you haven't seen any physical changes in supply at this point, don't stress. Monitor the baby's output and continue to feed frequently and stimulate every 2 to 3 hours. You should see changes in the next few days. If not, you should be seen by a lactation consultant to assess the situation.
Very important! Mothers who have had breast reduction or other nipple surgery should be aware that they may never establish a full milk supply. There are methods to maximize what they can make, but the promise of a full supply cannot be made.
Tips
Keep plugging away! Sore nipples, sleepy babies -- it will all subside within the next week if you're consistent about proper latch-ons and frequent feedings.
Some breast discomfort will probably make its appearance as your milk comes in. However, with frequent feedings you can avoid severe engorgement. So try your best to be persistent and consistent to avoid the problem.
<Support Us via "Like" our facebok Page and Share>
Scene 1: The Hospital. You have just delivered a beautiful, perfect baby. He sleeps like an angel in the nursery, in your room. You gloat to all friends and family about your wonderful feeder and sleeper. A few days later, you are discharged and take him home.
Scene 2: Home, Day 3. The honeymoon is over...Your baby is feeding frequently and for long periods of time. His sleep patterns have miraculously changed and he is awake all night, crying more often. You feel, "What have I done wrong? He was so perfect in the hospital!" The answer is: Absolutely nothing! This is, fortunately or unfortunately, normal.
What to Generally Expect at This Stage
Whether a baby is exhausted from the long journey into this world, sleeping heavily because of the hum of activity in the nursery or because he is being held against your warm body, babies generally sleep well in the hospital. (Moms who have had C-sections are often more realistic in their expectations once they go home because they are in the hospital a bit longer, which means that their babies "wake up" while they're in the hospital.) Once they come home, everything changes: Feedings are much more frequent and last longer and sleep patterns adjust because of the new schedule. Some babies feed for what may seem like hours and then sleep for many hours. Once the milk comes in, patterns change yet again!
Common Issues For Mother at This Stage
Aside from physical exhaustion kicking in, sore nipples continue to be the most common issue in the first three days postpartum. At this stage, even with a properly latched baby, nipple sensitivity is still prevalent because of postpartum hormonal changes. However, if nipples are cracked, bleeding, or blistering, the latch-on needs help. Contact a lactation consultant immediately.
Some moms also find that their milk has started to transition from colostrum to transitional milk by Day 3. They often feel a heaviness to their breasts, which indicates that their milk is starting to "come in." Feeding frequently will combat any discomfort.
Common Issues For Baby at This Stage
Jaundice is common in breastfed babies. However, by breastfeeding frequently (at least 8 to 10 times a day) in the first 3 days of life, you can greatly reduce the chances that your baby will require higher intervention, such as phototherapy (going under bilirubin lights.)
Sleepiness may also prevail...
Waking Up A Sleepy Baby
Your body is in the process of building a milk supply that will fully sustain your baby and your baby needs frequent feedings for her growth and development. It is essential for both the establishment of your milk supply and the baby's nutrition to continue to wake the baby if he is not waking himself. Some people or books may tell you that you should never wake a sleeping baby. While that may be true later -- after your milk supply is established and the baby is showing all signs of feeding well -- at this stage it is very important.
Establishing A Milk Supply
At this stage, you will notice your breasts becoming fuller and heavier. Your milk is "coming in!" Your milk is changing from colostrum to transitional milk and you will notice the color changing from a clear, yellowish fluid (colostrum) to a thicker white (transitional milk). Continue to breastfeed (or, if necessary, pump) every 2 to 3 hours to stimulate supply.
If you haven't seen any physical changes in supply at this point, don't stress. Monitor the baby's output and continue to feed frequently and stimulate every 2 to 3 hours. You should see changes in the next few days. If not, you should be seen by a lactation consultant to assess the situation.
Very important! Mothers who have had breast reduction or other nipple surgery should be aware that they may never establish a full milk supply. There are methods to maximize what they can make, but the promise of a full supply cannot be made.
Tips
Keep plugging away! Sore nipples, sleepy babies -- it will all subside within the next week if you're consistent about proper latch-ons and frequent feedings.
Some breast discomfort will probably make its appearance as your milk comes in. However, with frequent feedings you can avoid severe engorgement. So try your best to be persistent and consistent to avoid the problem.
Seamless wireless comfort breastfeeding / MATERNITY bra with REMOVABLE padDING
Specially design just for you the perfect breastfeeding / maternity bra, you will be able to easily breastfeed your baby while providing comfortable support for yourself.
Product Feature:-
1) Wire-free breastfeeding / maternity bra
2) No hooks or clasps
3) Perfect seamless design
4) Comfort for sleeping with during nursing stages
5) Convenient for nursing with a convenient front closure
6) Exquisite subtle center bust shaping
7) Included removable padding for additional bust lift
8) Four-ways knitted fabric ribbed band for a cozy fit
9) Elastic spaghetti shoulder straps for flexible control and Convenient pull-on style
10) Breathable fabric makes you comfort and dry all day
11) Machine washable and easy to clean
12) 5 sizes and 2 colors for your choice
13) Material : 90% Nylon & 10% Spandex
Color : Black and Nude
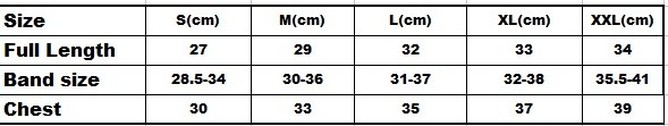
Size : S M L XL XXL XXXL
Retail Price : SGD 39.90 per piece
Product Feature:-
1) Wire-free breastfeeding / maternity bra
2) No hooks or clasps
3) Perfect seamless design
4) Comfort for sleeping with during nursing stages
5) Convenient for nursing with a convenient front closure
6) Exquisite subtle center bust shaping
7) Included removable padding for additional bust lift
8) Four-ways knitted fabric ribbed band for a cozy fit
9) Elastic spaghetti shoulder straps for flexible control and Convenient pull-on style
10) Breathable fabric makes you comfort and dry all day
11) Machine washable and easy to clean
12) 5 sizes and 2 colors for your choice
13) Material : 90% Nylon & 10% Spandex
Color : Black and Nude
Size : S M L XL XXL XXXL
Retail Price : SGD 39.90 per piece
Exclusive Pumping – The Best… Expressed!
A note about exclusive pumping:
There are occasions that arise which may prevent a mom from being able to nurse her baby. A mother who has a baby who cannot or will not latch, for whatever reason, may assume there is no choice but for her to use infant formula. There is another option however, and one that doesn’t seem to get the support or acknowledgment it deserves – exclusively pumping, also known as “EPing“.
In most cases, a mother who has made the decision to exclusively pump has not done so “lightly”. She is aware of the irreplaceable benefits of her milk, and she wants her baby to have the best, so the most logical conclusion for her is to pump and provide her milk to baby by bottle.
Sadly, many (including health care providers) will tell mom that this is crazy idea, and “it’ll never work”; “you’ll run out of milk”; or will say “you simply will not be able to keep up”. Without the support and information she
needs, a mom may simply give up.
Those who don’t give up often are faced with other issues to overcome. They often feel like they are in a class by themselves, excluded from the usual groups of moms who typically form into “support groups” either for breastfeeding mothers, or for formula feeding mothers.
They may feel they must explain “why” they are “bottle feeding” breastmilk – even to their health care providers who often ask.. “breast or bottle” assuming “bottle” is formula.
While everyone does agree that there are irreplaceable benefits to nursing baby directly from breast, everyone also must agree that breastmilk itself is irreplaceable. When faced with providing breastmilk, or not, then whenever possible it should be breastmilk regardless of the method of delivery.
There is no room or need for guilt here – the mother who has done all she can to bf “normally” isn’t a failure – she is just doing the best she can in the situation she is in. Mothers who choose to exclusively pump are very dedicated mothers – determined to do the best they can for their precious babies, and they deserve respect and support.
Here are some tips and information regarding exclusive pumping:
All About Exclusive Pumping and Tips for EPing Moms by EPing Moms
(italicized info shared by Shanna)
HOW OFTEN TO PUMP & WHEN?:
First and foremost – one should have a good quality, double electric pump. Some mothers rent them, others buy pumps such as the Hygeia EnJoye. The quality of the pump can make all the difference in the world!
A normal newborn baby nurses on average 8 to 12 times in a 24 hour period. Most experts suggest it is best if mom can come close to matching what the normal nursing baby would do at the breast, and recommend she pump about every two hours, not going longer than three hours between sessions. Understanding how
milk production works can help moms in their efforts to establish good milk supply. The more frequently the breasts are emptied, the more milk mother should have. Therefore, if she were to pump at least every 3 hours, for about 20 minutes, she should establish and maintain a good milk supply. In the first couple of weeks, she may also want to pump at least twice at night, but not all mothers do this.
“It’s insanely hard in the beginning but you need to pump every 2 to 3
hours around the clock. Prolactin levels (the hormone that tells your body to
make milk) are highest in the early morning hours so mom would want to make sure
she is pumping then as well. This is like the 1am to 5am stretch of time. If mom
can at least get one pump in during this time, it will really help.
The main concern is to get enough pumps in per day – a minimum of 7 pumps
per day. I will say from experience that when I pushed myself to get in 8 pumps
per day, my supply REALLY increased. Most of the time, I just couldn’t push
myself and ended up with 7 times. And to create a little bit of sanity, it is
the number of pumps per day that you get in and not necessarily the amount of
time you wait in between pumps that counts. So, if I needed to run an errand or
just wanted to get out of the house without dragging my pump along, I would pump
every 2 hours in the morning and then have a window of about 4 or 5 hours in the
afternoon to do everything and would then pump again every 2 hours in the
evening to get my total of 7 pumps in for the day.
That being said, I did NOT get up to pump in the middle of the night if
my baby wasn’t awake. I thought that was cruel and couldn’t do it! Ha! The sleep
was more important to me (especially after the c-section). A lot of pumping is
trial and error and this is why keeping info in a spreadsheet (or journal) is
helpful. If you start sleeping through the night or going longer stretches and
see a huge decline in your volume, you can always set you alarm to add another
pump back in. I never had to but this can vary from mom to mom. I did the early
morning pump as long as I was up feeding the baby, but if she slept 5 hours
through the night, so did I! ”
PUMPING – HOW LONG?
Most experts agree that whatever the reason for pumping, moms should pump for about 20 minutes. Most agree its best to pump at least 15 minutes, and to avoid going much longer than 20 minutes. Experts also encourage pumping about five minutes past when the milk stops flowing, often by doing so mom will elicit
another letdown, and at the very least will maintain production as well as encouraging increase in supply if needed.
“The standard advice is to pump for 15-20 minutes. Even if you don’t have
milk flowing that entire time, you need to pump that long to get enough nipple
stimulation. Also pumping at least 5 minutes after your milk stops flowing will
tell your body that you need more milk; thus increasing your supply. 15 minutes
should absolutely be the minimum pumping time. I’ve talked to women who only
pumped for 10 minutes and eventually started losing their supply. They had to
work really hard to rebuild it.”
Pump Settings
“More is not better” when it comes to the suction settings on the breast pump. Most experienced moms do not set the pump speed on high, but rather keep it on lower setting for comfort.
“This one was a BIGGIE for me and I want to definitely pass this one on!
There should be a suction setting on your pump and a speed dial. This is very
important, the higher the suction does NOT mean the more milk you make. Your
pump will probably have a suction setting of minimum, medium, and maximum. I had
mine set on medium when I developed a blister. Once it healed, I turned it down
to minimum and have never had another blister or pain again. I keep the speed at
3 but if you feel like too much areola is being sucked into the horn, then
turning down the speed will remedy that. If you are in a lot of pain and turn
down the settings, you might actually get more milk because you are more
relaxed!”
HOW MUCH MILK PER BOTTLE?
Moms may find it surprising that the breastfed baby often takes less milk in the bottle than formula babies take in. This is because breastmilk is so well utilized by the baby’s body that less is needed. Since breastmilk is so easily and completely digested, the breastfed baby needs to eat more often, but they don’t need as much per bottle.
When a baby is nursed from the breast, research shows us that baby will vary
their intake of milk from feeding to feeding, and the length of time at the
breast doesn’t always correlate with the amount of milk taken from the breast.
Overall, the average bf baby takes in between 19 and 30 oz (or 570 – 900 mL) per
day (24 hrs), but the amount taken per bottle may vary somewhat from feeding to
feeding, just as it does at the breast, depending on baby’s need at the
time.
” According to the most current breastfeeding research, exclusively breastfed
babies take in an average of 25 oz (750 mL) per day between the ages of 1 month
and 6 months. This may vary a little from baby to baby, but the average range of
milk intake is 19-30 oz per day (570-900 mL per day).
To estimate the average amount of milk baby will need at a feeding:
This gives you a “ballpark” figure for the amount of expressed milk your exclusively breastfed baby will need at one feeding.
Example: If baby usually nurses around 8 times per day, you can guess that baby might need around 3 ounces per feeding every 3 hours when mom is away. (25/8=3.1).
NOTE: Current breastfeeding research does not indicate that breastmilk intake changes with baby’s age or weight between one and six months.”
HOW TO BOTTLE FEED
It is important to remember that it is very easy to overfeed a baby using bottles. This is because the way a baby drinks from a bottle is very different than how a baby would nurse from the breast. A baby cannot control the flow of milk from a bottle thus experts recommend using slow flow or “newborn” type
nipples, to reduce the risk of overfeeding.
The breastmilk should never be warmed in the microwave, since doing so not only creates hot spots that cannot fully be distributed evenly even when the milk is mixed (the heat adheres to the fats which “glob” together, and can result in scalding of a baby’s mouth and throat), but it actually alters the composition of the breastmilk, damaging some of the nutrients. Shaking breastmilk is also not recommended (gently swirl to mix, instead).
Ideally bottlefeeding the baby should mimic how a mother breastfeeds her baby. The baby should be fed on cue, or demand, and not according to a rigid schedule. Breastmilk digests in about 90 minutes, so one
would expect the feedings to be anywhere from 1.5 hrs to 3 hours apart. (younger babies often need to eat more frequently than older babies).
The bottle should be offered gently, in a non-stressful manner, with the baby drawing the nipple into the mouth. The type of bottle or nipple is not as important as the manner in which the bottle is offered. A typical nursing session lasts about 15 to 20 min, and care should be taken to allow baby to take his/her time to drink the bottle, not “rushing” through a feeding as quickly as possible. Changing position mid-way through a feeding is often recommended, as is holding baby is a more upright position. Propping a bottle is also not
recommended.
INCREASING YOUR SUPPLY
There are wonderful tips on increasing milk supply below – those that work for nursing mothers also work for mothers who exclusively pump, the biggest “difference” is that nursing mothers are encouraged to put baby to breast often, and pumping mothers are encouraged to pump often. Probably THE most important thing to remember is to pump often and pump long enough to soften (or “empty”) the breast.
“Some little tips to help increase your supply if you really need it.
It’s nice to have these on hand just in case:
First drink plenty of water.
I don’t drink a ton but I make sure to stay hydrated. Check your pee when you go (I know, sounds funny!). If it is light yellow to clear, you are plenty hydrated.
Make sure you eat!
While you are pumping, you will keep the weight off, I promise! It can make you hungry as a horse and it does that for a reason. You need the extra calories because you are burning so much off! When I didn’t eat enough, I would get really light headed and feel like I was going to drop my baby…not good! Eventually, your hunger should taper off (mine has).
Eat REAL oatmeal, not the instant.
You can eat the quick oats (the ones that cook in 1 minute) or the old fashioned oats (that cook in 5 minutes). You can also make cookies that have oatmeal in them and get oatmeal
that way (I prefer this way! Ha!). The way they process the instant oatmeal, it doesn’t give you the same results. No one is sure how the oatmeal works but it does!
Get some rest
(yeah, I know easier said than done!) If you are exhausted and have the opportunity to take a nap (even if it pushes your pump back) do it! You will actually get more milk that way! Even if you’re not leeping, rest by sitting down a lot. Conserving energy is important.
Don’t stress too much.
This all depends on how you personally handle stress. I tend to be a thinker, so I think things out a lot.
It has to be some MAJOR stressful situation for it to hurt my supply.
Some suggest drinking dark beer, with or without alcohol.
Some say it’s the barley in it or something, that helps to increase supply. Plus some women just swear by the relaxation it gives them! You can have 1 or 2 beers without much crossing into your milk.
(Note: Most breastfeeding experts do not routinely recommend using alcohol to boost
milk supply. )
There is a tea and it is supposed to help you increase your supply if you drink it.
There are herbs like Fenugreek and also prescription medications that will increase your supply if you really need it. I would use these as a last resort but they can be effective and are available!
Most importantly, good pumping habits will keep your supply up and increase it!”
PUMPING TRICKS & More Tips For EPing Moms by EPing Moms
(aka “Tricks of the Trade” shared by Shanna)
“Go hands free!
This was the best trick I learned!!
I went hands free and set my pump up by my computer and read my pumping board while I pump. It keeps me from looking down into my bottles wondering how much I’m getting, being bored out of my mind, and makes time FLY by! You can use an old nursing bra and just cut slits in the flap. Then you just slide the horns through. I did this for a while but I didn’t want to wear the cut up bra all day long so that meant I had to literally change bras before each pump. At 7 times a day, that was a bit much!! So, I bought a pumping bra and LOVE it! It’s the Easy
Expressions bustier.
The best thing about this bustier is that it can be worn over any nursing bra. So, when it’s time to pump, I put the flaps down on my nursing bra, wrap the bustier around, slide the horns through the holes, position them and zip it up. That’s all!”
“The refrigerator trick.
This is where you rinse your horns and/or collection bottles after each pumping session. You put them in a
ziplock bag (or not, this is optional), and put them in the refrigerator. The idea is that since breast milk is good in the fridge for 5-8 days, any residue left on the horns won’t matter. Then you can wash the horns/bottles once at
night. I throw mine into the dishwasher (all except the white membranes) and it’s easy, easy, easy!”
“Storage bags.
Many of us started out using the Gerber Seal-N-Go bag but they get very pricey quickly. They are like $5.50 for a box of 25 bags. After researching it online, I found many other women were using regular freezer bags for freezing the milk….MUCH cheaper! Everything I’ve read shows that they are safe to use. From what I have found, I only buy Glad and not Ziploc. Ziploc seems to have a much higher rate of leaks. I write the date and amount of ounces on the label with a sharpie and put the milk in and freeze flat. I then take several of them and put them into a gallon size freezer bag and write the dates that are enclosed on the gallon bag. This helps by double bagging and keeping them grouped. This way the corners on the bags won’t get poked and possibly cause the bag to leak. Also, whenever I want to get a bag, I can just dig through gallon size bags instead of tons of little bags floating around! : I usually put one or two days worth in a gallon bag.”
“Lube Up!
It is perfectly safe to put the lansinoh on before pumping and still use the milk. Putting it on before and after pumping really helps to keep you from getting too sore. Purelan100 is also good (and cheaper). I’ve used this from the beginning. You can also rub Olive Oil on the horns and inside the nipple chamber to reduce friction. Olive Oil is
antibacterial so it is helpful. This is also safe to use and pump milk with. I’ve done both of these and hadn’t had a problem. There are times when I seem to get sorer than other times with no real explanation. But, it then goes away as quickly as it came! Who knows!”
“Taking Care of Baby When Pumping.
Once I went hands free and had to do those early morning feedings by myself, I would sit on the floor and prop my baby up in her boppy pillow on the floor. I would get hooked up to the pump and start it and pump while I fed her. About the time she was done eating, I was done pumping and I would put her back in bed and go to sleep
myself. This will cut down on your time tremendously! It also helps to do this if your pumping time happens to correspond to your baby’s feeding time during the day. The bouncy seat is my best friend! I would put her in the bouncy seat and bounce it with my foot while surfing the net and pumping. It made time fly by and she was content. You may find other solutions if you have older children, or extra help.”
“Taking Care of Older Children, and Pumping.
You may not need a lot of tricks for this one depending on the age of the child, or children. They will probably understand if you just explain that while you are pumping, they can’t get up and get things without help. Some tricks other moms had mentioned to keep their other child entertained and kind of reward them would be to go shopping and let your child pick out a special toy or video that she really wants. Then when ever it comes time for you to pump, she can play with it. But, she ONLY gets to play with it when you pump. This helps to make pumping time special for her as well and can help prevent any resentment she might begin to feel.”
“Warnings:
Excessive caffeine may cause problems (like keeping the baby wired!). I avoid caffeine completely (except chocolate) but even if you have 1 drink a day, it won’t hurt. Just don’t go over board.
Medications that have Sudafed (pseudoephedrine HCl) in them can affect milk supply! Be careful!
Regular birth control pills will impact milk supply, and some women even have a problem with the mini pill. Breastfeeding (and yes that’s what you are doing even if it’s not from “the tap”) is a good deterrent for
ovulation but not 100% so be careful! However, you may find you get hot flashes and things like that. It is normal because your body is acting like it’s going through menopause. This suppresses ovulation and allows you to make milk. I thought I was going crazy until I learned this! Ha! Sometimes if you get your
period back while pumping, it can decrease your supply. This can be fixed by taking a calcium/magnesium supplement. (I don’t have mine back yet and loving it!).
“WHEN DOES THIS GET EASIER?
Around 3 months your supply will probably be established. This is when you can begin to drop the number of times per day that you pump and not see too much of a decrease in total output (this is again, where the spreadsheet comes in handy). That’s why if you do the hard work in the beginning, I promise it will pay off when this time comes! If you don’t keep up the number of pumps per day in the beginning, you may continue to have to pump a high number of times per day just to maintain a small supply. Of course, this is all dependent on how each woman produces milk. So, you may have such a great supply and so much frozen that you can drop pumps earlier. I began dropping pumps at 10 weeks and by 3 months I was down to 4 pumps per day! I lost a little with each drop but am currently at 50 ounces per day. There’s no way my baby will ever eat that much so I see no reason to pump more. You will have to decide for yourself. Once you start dropping pumps, you will need to pump longer at each session (because you’ve gone longer in between pumps and need longer to empty your breasts). This is also dependent on the woman. I pump about 35-40
minutes per pump now on 4 times because I get another let down at about 36 minutes into it!”
“YOU CAN DO THIS!!!
I firmly believe that pumping is 10% physical and 90% psychological. If you try to view this as positively as possible, I think you will have a better outcome. That’s why going hands free and doing everything to minimize your stress about pumping is important.
A lot of people don’t understand pumping. I still get stupid questions like, “Why don’t you just nurse?” Well, DUH! She won’t nurse! Ha! You should do whatever makes you comfortable. Sometimes strangers ask me if I’m breastfeeding and if I don’t feel like dealing with anything, I just say yes. I am after all! She’s just getting it “to go” instead of from “the tap”! Ha!
Mostly though, I do all I can to educate. I know many women who didn’t know this option was even possible and wished they had when breastfeeding didn’t work out. Don’t listen to doctors or nurses who tell you this isn’t possible. There just isn’t enough wide spread info out there and unfortunately most health care professionals give really bad advice (like only pump for 10 minutes). So, when they hear back from their patients on how they had supply problems or dried up, they just assume it’s not possible to pump long term. On my online group, there are women who have been pumping for a year or longer! It is DEFINITELY possible!
Most importantly, if for any reason you just don’t want to do it anymore, it is perfectly fine! Remember, a happy mommy = a happy baby. You have to do whatever is right for your entire family. Pumping is hard and can take its toll on you. There is no right or wrong when it comes to how you feed your baby! Remember that! We all have days when we want to wean. That’s why support is SOOO important!
There are occasions that arise which may prevent a mom from being able to nurse her baby. A mother who has a baby who cannot or will not latch, for whatever reason, may assume there is no choice but for her to use infant formula. There is another option however, and one that doesn’t seem to get the support or acknowledgment it deserves – exclusively pumping, also known as “EPing“.
In most cases, a mother who has made the decision to exclusively pump has not done so “lightly”. She is aware of the irreplaceable benefits of her milk, and she wants her baby to have the best, so the most logical conclusion for her is to pump and provide her milk to baby by bottle.
Sadly, many (including health care providers) will tell mom that this is crazy idea, and “it’ll never work”; “you’ll run out of milk”; or will say “you simply will not be able to keep up”. Without the support and information she
needs, a mom may simply give up.
Those who don’t give up often are faced with other issues to overcome. They often feel like they are in a class by themselves, excluded from the usual groups of moms who typically form into “support groups” either for breastfeeding mothers, or for formula feeding mothers.
They may feel they must explain “why” they are “bottle feeding” breastmilk – even to their health care providers who often ask.. “breast or bottle” assuming “bottle” is formula.
While everyone does agree that there are irreplaceable benefits to nursing baby directly from breast, everyone also must agree that breastmilk itself is irreplaceable. When faced with providing breastmilk, or not, then whenever possible it should be breastmilk regardless of the method of delivery.
There is no room or need for guilt here – the mother who has done all she can to bf “normally” isn’t a failure – she is just doing the best she can in the situation she is in. Mothers who choose to exclusively pump are very dedicated mothers – determined to do the best they can for their precious babies, and they deserve respect and support.
Here are some tips and information regarding exclusive pumping:
All About Exclusive Pumping and Tips for EPing Moms by EPing Moms
(italicized info shared by Shanna)
HOW OFTEN TO PUMP & WHEN?:
First and foremost – one should have a good quality, double electric pump. Some mothers rent them, others buy pumps such as the Hygeia EnJoye. The quality of the pump can make all the difference in the world!
A normal newborn baby nurses on average 8 to 12 times in a 24 hour period. Most experts suggest it is best if mom can come close to matching what the normal nursing baby would do at the breast, and recommend she pump about every two hours, not going longer than three hours between sessions. Understanding how
milk production works can help moms in their efforts to establish good milk supply. The more frequently the breasts are emptied, the more milk mother should have. Therefore, if she were to pump at least every 3 hours, for about 20 minutes, she should establish and maintain a good milk supply. In the first couple of weeks, she may also want to pump at least twice at night, but not all mothers do this.
“It’s insanely hard in the beginning but you need to pump every 2 to 3
hours around the clock. Prolactin levels (the hormone that tells your body to
make milk) are highest in the early morning hours so mom would want to make sure
she is pumping then as well. This is like the 1am to 5am stretch of time. If mom
can at least get one pump in during this time, it will really help.
The main concern is to get enough pumps in per day – a minimum of 7 pumps
per day. I will say from experience that when I pushed myself to get in 8 pumps
per day, my supply REALLY increased. Most of the time, I just couldn’t push
myself and ended up with 7 times. And to create a little bit of sanity, it is
the number of pumps per day that you get in and not necessarily the amount of
time you wait in between pumps that counts. So, if I needed to run an errand or
just wanted to get out of the house without dragging my pump along, I would pump
every 2 hours in the morning and then have a window of about 4 or 5 hours in the
afternoon to do everything and would then pump again every 2 hours in the
evening to get my total of 7 pumps in for the day.
That being said, I did NOT get up to pump in the middle of the night if
my baby wasn’t awake. I thought that was cruel and couldn’t do it! Ha! The sleep
was more important to me (especially after the c-section). A lot of pumping is
trial and error and this is why keeping info in a spreadsheet (or journal) is
helpful. If you start sleeping through the night or going longer stretches and
see a huge decline in your volume, you can always set you alarm to add another
pump back in. I never had to but this can vary from mom to mom. I did the early
morning pump as long as I was up feeding the baby, but if she slept 5 hours
through the night, so did I! ”
PUMPING – HOW LONG?
Most experts agree that whatever the reason for pumping, moms should pump for about 20 minutes. Most agree its best to pump at least 15 minutes, and to avoid going much longer than 20 minutes. Experts also encourage pumping about five minutes past when the milk stops flowing, often by doing so mom will elicit
another letdown, and at the very least will maintain production as well as encouraging increase in supply if needed.
“The standard advice is to pump for 15-20 minutes. Even if you don’t have
milk flowing that entire time, you need to pump that long to get enough nipple
stimulation. Also pumping at least 5 minutes after your milk stops flowing will
tell your body that you need more milk; thus increasing your supply. 15 minutes
should absolutely be the minimum pumping time. I’ve talked to women who only
pumped for 10 minutes and eventually started losing their supply. They had to
work really hard to rebuild it.”
Pump Settings
“More is not better” when it comes to the suction settings on the breast pump. Most experienced moms do not set the pump speed on high, but rather keep it on lower setting for comfort.
“This one was a BIGGIE for me and I want to definitely pass this one on!
There should be a suction setting on your pump and a speed dial. This is very
important, the higher the suction does NOT mean the more milk you make. Your
pump will probably have a suction setting of minimum, medium, and maximum. I had
mine set on medium when I developed a blister. Once it healed, I turned it down
to minimum and have never had another blister or pain again. I keep the speed at
3 but if you feel like too much areola is being sucked into the horn, then
turning down the speed will remedy that. If you are in a lot of pain and turn
down the settings, you might actually get more milk because you are more
relaxed!”
HOW MUCH MILK PER BOTTLE?
Moms may find it surprising that the breastfed baby often takes less milk in the bottle than formula babies take in. This is because breastmilk is so well utilized by the baby’s body that less is needed. Since breastmilk is so easily and completely digested, the breastfed baby needs to eat more often, but they don’t need as much per bottle.
When a baby is nursed from the breast, research shows us that baby will vary
their intake of milk from feeding to feeding, and the length of time at the
breast doesn’t always correlate with the amount of milk taken from the breast.
Overall, the average bf baby takes in between 19 and 30 oz (or 570 – 900 mL) per
day (24 hrs), but the amount taken per bottle may vary somewhat from feeding to
feeding, just as it does at the breast, depending on baby’s need at the
time.
” According to the most current breastfeeding research, exclusively breastfed
babies take in an average of 25 oz (750 mL) per day between the ages of 1 month
and 6 months. This may vary a little from baby to baby, but the average range of
milk intake is 19-30 oz per day (570-900 mL per day).
To estimate the average amount of milk baby will need at a feeding:
- Estimate the number of times that baby nurses per day (24 hours).
- Then divide 25 oz by the number of nursings.
This gives you a “ballpark” figure for the amount of expressed milk your exclusively breastfed baby will need at one feeding.
Example: If baby usually nurses around 8 times per day, you can guess that baby might need around 3 ounces per feeding every 3 hours when mom is away. (25/8=3.1).
NOTE: Current breastfeeding research does not indicate that breastmilk intake changes with baby’s age or weight between one and six months.”
HOW TO BOTTLE FEED
It is important to remember that it is very easy to overfeed a baby using bottles. This is because the way a baby drinks from a bottle is very different than how a baby would nurse from the breast. A baby cannot control the flow of milk from a bottle thus experts recommend using slow flow or “newborn” type
nipples, to reduce the risk of overfeeding.
The breastmilk should never be warmed in the microwave, since doing so not only creates hot spots that cannot fully be distributed evenly even when the milk is mixed (the heat adheres to the fats which “glob” together, and can result in scalding of a baby’s mouth and throat), but it actually alters the composition of the breastmilk, damaging some of the nutrients. Shaking breastmilk is also not recommended (gently swirl to mix, instead).
Ideally bottlefeeding the baby should mimic how a mother breastfeeds her baby. The baby should be fed on cue, or demand, and not according to a rigid schedule. Breastmilk digests in about 90 minutes, so one
would expect the feedings to be anywhere from 1.5 hrs to 3 hours apart. (younger babies often need to eat more frequently than older babies).
The bottle should be offered gently, in a non-stressful manner, with the baby drawing the nipple into the mouth. The type of bottle or nipple is not as important as the manner in which the bottle is offered. A typical nursing session lasts about 15 to 20 min, and care should be taken to allow baby to take his/her time to drink the bottle, not “rushing” through a feeding as quickly as possible. Changing position mid-way through a feeding is often recommended, as is holding baby is a more upright position. Propping a bottle is also not
recommended.
INCREASING YOUR SUPPLY
There are wonderful tips on increasing milk supply below – those that work for nursing mothers also work for mothers who exclusively pump, the biggest “difference” is that nursing mothers are encouraged to put baby to breast often, and pumping mothers are encouraged to pump often. Probably THE most important thing to remember is to pump often and pump long enough to soften (or “empty”) the breast.
“Some little tips to help increase your supply if you really need it.
It’s nice to have these on hand just in case:
First drink plenty of water.
I don’t drink a ton but I make sure to stay hydrated. Check your pee when you go (I know, sounds funny!). If it is light yellow to clear, you are plenty hydrated.
Make sure you eat!
While you are pumping, you will keep the weight off, I promise! It can make you hungry as a horse and it does that for a reason. You need the extra calories because you are burning so much off! When I didn’t eat enough, I would get really light headed and feel like I was going to drop my baby…not good! Eventually, your hunger should taper off (mine has).
Eat REAL oatmeal, not the instant.
You can eat the quick oats (the ones that cook in 1 minute) or the old fashioned oats (that cook in 5 minutes). You can also make cookies that have oatmeal in them and get oatmeal
that way (I prefer this way! Ha!). The way they process the instant oatmeal, it doesn’t give you the same results. No one is sure how the oatmeal works but it does!
Get some rest
(yeah, I know easier said than done!) If you are exhausted and have the opportunity to take a nap (even if it pushes your pump back) do it! You will actually get more milk that way! Even if you’re not leeping, rest by sitting down a lot. Conserving energy is important.
Don’t stress too much.
This all depends on how you personally handle stress. I tend to be a thinker, so I think things out a lot.
It has to be some MAJOR stressful situation for it to hurt my supply.
Some suggest drinking dark beer, with or without alcohol.
Some say it’s the barley in it or something, that helps to increase supply. Plus some women just swear by the relaxation it gives them! You can have 1 or 2 beers without much crossing into your milk.
(Note: Most breastfeeding experts do not routinely recommend using alcohol to boost
milk supply. )
There is a tea and it is supposed to help you increase your supply if you drink it.
There are herbs like Fenugreek and also prescription medications that will increase your supply if you really need it. I would use these as a last resort but they can be effective and are available!
Most importantly, good pumping habits will keep your supply up and increase it!”
PUMPING TRICKS & More Tips For EPing Moms by EPing Moms
(aka “Tricks of the Trade” shared by Shanna)
“Go hands free!
This was the best trick I learned!!
I went hands free and set my pump up by my computer and read my pumping board while I pump. It keeps me from looking down into my bottles wondering how much I’m getting, being bored out of my mind, and makes time FLY by! You can use an old nursing bra and just cut slits in the flap. Then you just slide the horns through. I did this for a while but I didn’t want to wear the cut up bra all day long so that meant I had to literally change bras before each pump. At 7 times a day, that was a bit much!! So, I bought a pumping bra and LOVE it! It’s the Easy
Expressions bustier.
The best thing about this bustier is that it can be worn over any nursing bra. So, when it’s time to pump, I put the flaps down on my nursing bra, wrap the bustier around, slide the horns through the holes, position them and zip it up. That’s all!”
“The refrigerator trick.
This is where you rinse your horns and/or collection bottles after each pumping session. You put them in a
ziplock bag (or not, this is optional), and put them in the refrigerator. The idea is that since breast milk is good in the fridge for 5-8 days, any residue left on the horns won’t matter. Then you can wash the horns/bottles once at
night. I throw mine into the dishwasher (all except the white membranes) and it’s easy, easy, easy!”
“Storage bags.
Many of us started out using the Gerber Seal-N-Go bag but they get very pricey quickly. They are like $5.50 for a box of 25 bags. After researching it online, I found many other women were using regular freezer bags for freezing the milk….MUCH cheaper! Everything I’ve read shows that they are safe to use. From what I have found, I only buy Glad and not Ziploc. Ziploc seems to have a much higher rate of leaks. I write the date and amount of ounces on the label with a sharpie and put the milk in and freeze flat. I then take several of them and put them into a gallon size freezer bag and write the dates that are enclosed on the gallon bag. This helps by double bagging and keeping them grouped. This way the corners on the bags won’t get poked and possibly cause the bag to leak. Also, whenever I want to get a bag, I can just dig through gallon size bags instead of tons of little bags floating around! : I usually put one or two days worth in a gallon bag.”
“Lube Up!
It is perfectly safe to put the lansinoh on before pumping and still use the milk. Putting it on before and after pumping really helps to keep you from getting too sore. Purelan100 is also good (and cheaper). I’ve used this from the beginning. You can also rub Olive Oil on the horns and inside the nipple chamber to reduce friction. Olive Oil is
antibacterial so it is helpful. This is also safe to use and pump milk with. I’ve done both of these and hadn’t had a problem. There are times when I seem to get sorer than other times with no real explanation. But, it then goes away as quickly as it came! Who knows!”
“Taking Care of Baby When Pumping.
Once I went hands free and had to do those early morning feedings by myself, I would sit on the floor and prop my baby up in her boppy pillow on the floor. I would get hooked up to the pump and start it and pump while I fed her. About the time she was done eating, I was done pumping and I would put her back in bed and go to sleep
myself. This will cut down on your time tremendously! It also helps to do this if your pumping time happens to correspond to your baby’s feeding time during the day. The bouncy seat is my best friend! I would put her in the bouncy seat and bounce it with my foot while surfing the net and pumping. It made time fly by and she was content. You may find other solutions if you have older children, or extra help.”
“Taking Care of Older Children, and Pumping.
You may not need a lot of tricks for this one depending on the age of the child, or children. They will probably understand if you just explain that while you are pumping, they can’t get up and get things without help. Some tricks other moms had mentioned to keep their other child entertained and kind of reward them would be to go shopping and let your child pick out a special toy or video that she really wants. Then when ever it comes time for you to pump, she can play with it. But, she ONLY gets to play with it when you pump. This helps to make pumping time special for her as well and can help prevent any resentment she might begin to feel.”
“Warnings:
Excessive caffeine may cause problems (like keeping the baby wired!). I avoid caffeine completely (except chocolate) but even if you have 1 drink a day, it won’t hurt. Just don’t go over board.
Medications that have Sudafed (pseudoephedrine HCl) in them can affect milk supply! Be careful!
Regular birth control pills will impact milk supply, and some women even have a problem with the mini pill. Breastfeeding (and yes that’s what you are doing even if it’s not from “the tap”) is a good deterrent for
ovulation but not 100% so be careful! However, you may find you get hot flashes and things like that. It is normal because your body is acting like it’s going through menopause. This suppresses ovulation and allows you to make milk. I thought I was going crazy until I learned this! Ha! Sometimes if you get your
period back while pumping, it can decrease your supply. This can be fixed by taking a calcium/magnesium supplement. (I don’t have mine back yet and loving it!).
“WHEN DOES THIS GET EASIER?
Around 3 months your supply will probably be established. This is when you can begin to drop the number of times per day that you pump and not see too much of a decrease in total output (this is again, where the spreadsheet comes in handy). That’s why if you do the hard work in the beginning, I promise it will pay off when this time comes! If you don’t keep up the number of pumps per day in the beginning, you may continue to have to pump a high number of times per day just to maintain a small supply. Of course, this is all dependent on how each woman produces milk. So, you may have such a great supply and so much frozen that you can drop pumps earlier. I began dropping pumps at 10 weeks and by 3 months I was down to 4 pumps per day! I lost a little with each drop but am currently at 50 ounces per day. There’s no way my baby will ever eat that much so I see no reason to pump more. You will have to decide for yourself. Once you start dropping pumps, you will need to pump longer at each session (because you’ve gone longer in between pumps and need longer to empty your breasts). This is also dependent on the woman. I pump about 35-40
minutes per pump now on 4 times because I get another let down at about 36 minutes into it!”
“YOU CAN DO THIS!!!
I firmly believe that pumping is 10% physical and 90% psychological. If you try to view this as positively as possible, I think you will have a better outcome. That’s why going hands free and doing everything to minimize your stress about pumping is important.
A lot of people don’t understand pumping. I still get stupid questions like, “Why don’t you just nurse?” Well, DUH! She won’t nurse! Ha! You should do whatever makes you comfortable. Sometimes strangers ask me if I’m breastfeeding and if I don’t feel like dealing with anything, I just say yes. I am after all! She’s just getting it “to go” instead of from “the tap”! Ha!
Mostly though, I do all I can to educate. I know many women who didn’t know this option was even possible and wished they had when breastfeeding didn’t work out. Don’t listen to doctors or nurses who tell you this isn’t possible. There just isn’t enough wide spread info out there and unfortunately most health care professionals give really bad advice (like only pump for 10 minutes). So, when they hear back from their patients on how they had supply problems or dried up, they just assume it’s not possible to pump long term. On my online group, there are women who have been pumping for a year or longer! It is DEFINITELY possible!
Most importantly, if for any reason you just don’t want to do it anymore, it is perfectly fine! Remember, a happy mommy = a happy baby. You have to do whatever is right for your entire family. Pumping is hard and can take its toll on you. There is no right or wrong when it comes to how you feed your baby! Remember that! We all have days when we want to wean. That’s why support is SOOO important!
Breastfeeding - Starting Out Right
Breastfeeding is the natural, physiologic way of feeding infants and young
children milk, and human milk is the milk made specifically for human infants.
Formulas made from cow’s milk or soy beans (most of them) are only superficially
similar, and advertising which states otherwise is misleading. Breastfeeding
should be easy and trouble free for most mothers. A good start helps to assure
breastfeeding is a happy experience for both mother and baby.
The vast majority of mothers are perfectly capable of breastfeeding their
babies exclusively for four to six months. In fact, most mothers produce more
than enough milk. Unfortunately, outdated hospital routines based on bottle
feeding still predominate in many health care institutions and make
breastfeeding difficult, even impossible, for some mothers and babies. For
breastfeeding to be well and properly established, a good early few days can be
crucial. Admittedly, even with a terrible start, many mothers and babies
manage.
The trick to breastfeeding is getting the baby to latch on well. A baby who
latches on well, gets milk well. A baby who latches on poorly has difficulty
getting milk, especially if the supply is low. A poor latch is similar to giving
a baby a bottle with a nipple hole which is too small—the bottle is full of
milk, but the baby will not get much. When a baby is latching on poorly, he may
also cause the mother nipple pain. And if he does not get milk well, he will
usually stay on the breast for long periods, thus aggravating the pain. Here are
a few ways breastfeeding can be made easy:
1. The baby should be at the breast immediately after
birth. The vast majority of newborns can be put to breast within
minutes of birth. Indeed, research has shown that, given the chance, babies only
minutes old will often crawl up to the breast from the mother’s abdomen, and
start breastfeeding all by themselves. This process may take up to an hour or
longer, but the mother and baby should be given this time together to start
learning about each other. Babies who "self-attach" run into far fewer
breastfeeding problems. This process does not take any effort on the mother’s
part, and the excuse that it cannot be done because the mother is tired after
labour is nonsense, pure and simple. Incidentally, studies have also shown that
skin to skin contact between mothers and babies keeps the baby as warm as an
incubator.
2. The mother and baby should room in together. There is
absolutely no medical reason for healthy mothers and babies to be separated from
each other, even for short periods. Health facilities which have routine
separations of mothers and babies after birth are years behind the times, and
the reasons for the separation often have to do with letting parents know who is
in control (the hospital) and who is not (the parents). Often bogus reasons are
given for separations. One example is the baby passed meconium before birth. A
baby who passes meconium and is fine a few minutes after birth will be fine and
does not need to be in an incubator for several hours’ "observation".
There is no evidence that mothers who are separated from their babies are
better rested. On the contrary, they are more rested and less stressed when they
are with their babies. Mothers and babies learn how to sleep in the same rhythm.
Thus, when the baby starts waking for a feed, the mother is also starting to
wake up naturally. This is not as tiring for the mother as being awakened from
deep sleep, as she often is if the baby is elsewhere when he wakes up.
The baby shows long before he starts crying that he is ready to feed. His
breathing may change, for example. Or he may start to stretch. The mother, being
in light sleep, will awaken, her milk will start to flow and the calm baby will
be content to nurse. A baby who has been crying for some time before being tried
on the breast may refuse to take the breast even if he is ravenous. Mothers and
babies should be encouraged to sleep side by side in hospital. This is a great
way for mothers to rest while the baby nurses. Breastfeeding should be relaxing,
not tiring.
3. Artificial nipples should not be given to the baby. There
seems to be some controversy about whether "nipple confusion" exists. Babies
will take whatever method gives them a rapid flow of fluid and may refuse others
that do not. Thus, in the first few days, when the mother is producing only a
little milk (as nature intended), and the baby gets a bottle (as nature
intended?) from which he gets rapid flow, he will tend to prefer the rapid flow
method. You don’t have to be a rocket scientist to figure that one out, though
many health professionals, who are supposed to be helping you, don’t seem to be
able to manage it. Nipple confusion includes not just the baby refusing the
breast, but also the baby not taking the breast as well as he could and thus not
getting milk well and /or the mother getting sore nipples. Just because a baby
will "take both" does not mean that the bottle is not having a negative effect.
Since there are now alternatives available if the baby needs to be supplemented
why use an artificial nipple?
4. No restriction on length or frequency of breastfeedings.
A baby who drinks well will not be on the breast for hours at a time. Thus, if
he is, it is usually because he is not latching on well and not getting the milk
which is available. Get help to fix the baby’s latch, and use compression to get
the baby more milk. This, not a pacifier, not a
bottle, not taking the baby to the nursery, will help.
5. Supplements of water, sugar water, or formula are rarely
needed. Most supplements could be avoided by getting the baby to take
the breast properly and get the milk that is available. If you are being told
you need to supplement without someone having observed you breastfeeding, ask
for someone to help who knows what they are doing. There are rare indications
for supplementation, but usually supplements are suggested for the convenience
of the hospital staff. If supplements are required, they should be given by
lactation aid, not cup, finger feeding, syringe or
bottle. The best supplement is your own colostrum. It can be mixed with sugar
water if you are not able to express much at first. Formula is hardly ever
necessary in the first few days.
6. A proper latch is crucial to success. This is the key to
successful breastfeeding. Unfortunately, too many mothers are being "helped" by
people who don’t know what a proper latch is. If you are being told your two day
old’s latch is good despite your having very sore nipples, be skeptical, and ask
for help from someone who knows.
Before you leave the hospital, you should be shown that your baby is latched
on properly, and that he is actually getting milk from the breast and that you
know how to know he is getting milk from the breast (open—pause—close type of
suck). If you and the baby are leaving hospital not knowing this, get help
quickly.
7. Free formula samples and formula company literature are not
gifts. There is only one purpose for these "gifts" and that is to get
you to use formula. It is very effective, and very unethical, marketing. If you
get any from any health professional, you should be wondering about his/her
knowledge of breastfeeding and his/her commitment to breastfeeding. "But I need
formula because the baby is not getting enough!". Maybe, but, more likely, you
weren’t given good help and the baby is simply not getting your milk well. Get
good help. Formula samples are not help.
Under some circumstances, it may be impossible to start breastfeeding early.
However, most medical reasons (maternal medication, for example) are not true
reasons for stopping or delaying breastfeeding, and you are getting
misinformation. Get good help. Premature babies can start breastfeeding much,
much earlier than they do in many health facilities. In fact, studies are now
quite definite that it is easier for a premature baby to breastfeed than to
bottle feed. Unfortunately, too many health professionals dealing with premature
babies do not seem to be aware of this.
children milk, and human milk is the milk made specifically for human infants.
Formulas made from cow’s milk or soy beans (most of them) are only superficially
similar, and advertising which states otherwise is misleading. Breastfeeding
should be easy and trouble free for most mothers. A good start helps to assure
breastfeeding is a happy experience for both mother and baby.
The vast majority of mothers are perfectly capable of breastfeeding their
babies exclusively for four to six months. In fact, most mothers produce more
than enough milk. Unfortunately, outdated hospital routines based on bottle
feeding still predominate in many health care institutions and make
breastfeeding difficult, even impossible, for some mothers and babies. For
breastfeeding to be well and properly established, a good early few days can be
crucial. Admittedly, even with a terrible start, many mothers and babies
manage.
The trick to breastfeeding is getting the baby to latch on well. A baby who
latches on well, gets milk well. A baby who latches on poorly has difficulty
getting milk, especially if the supply is low. A poor latch is similar to giving
a baby a bottle with a nipple hole which is too small—the bottle is full of
milk, but the baby will not get much. When a baby is latching on poorly, he may
also cause the mother nipple pain. And if he does not get milk well, he will
usually stay on the breast for long periods, thus aggravating the pain. Here are
a few ways breastfeeding can be made easy:
1. The baby should be at the breast immediately after
birth. The vast majority of newborns can be put to breast within
minutes of birth. Indeed, research has shown that, given the chance, babies only
minutes old will often crawl up to the breast from the mother’s abdomen, and
start breastfeeding all by themselves. This process may take up to an hour or
longer, but the mother and baby should be given this time together to start
learning about each other. Babies who "self-attach" run into far fewer
breastfeeding problems. This process does not take any effort on the mother’s
part, and the excuse that it cannot be done because the mother is tired after
labour is nonsense, pure and simple. Incidentally, studies have also shown that
skin to skin contact between mothers and babies keeps the baby as warm as an
incubator.
2. The mother and baby should room in together. There is
absolutely no medical reason for healthy mothers and babies to be separated from
each other, even for short periods. Health facilities which have routine
separations of mothers and babies after birth are years behind the times, and
the reasons for the separation often have to do with letting parents know who is
in control (the hospital) and who is not (the parents). Often bogus reasons are
given for separations. One example is the baby passed meconium before birth. A
baby who passes meconium and is fine a few minutes after birth will be fine and
does not need to be in an incubator for several hours’ "observation".
There is no evidence that mothers who are separated from their babies are
better rested. On the contrary, they are more rested and less stressed when they
are with their babies. Mothers and babies learn how to sleep in the same rhythm.
Thus, when the baby starts waking for a feed, the mother is also starting to
wake up naturally. This is not as tiring for the mother as being awakened from
deep sleep, as she often is if the baby is elsewhere when he wakes up.
The baby shows long before he starts crying that he is ready to feed. His
breathing may change, for example. Or he may start to stretch. The mother, being
in light sleep, will awaken, her milk will start to flow and the calm baby will
be content to nurse. A baby who has been crying for some time before being tried
on the breast may refuse to take the breast even if he is ravenous. Mothers and
babies should be encouraged to sleep side by side in hospital. This is a great
way for mothers to rest while the baby nurses. Breastfeeding should be relaxing,
not tiring.
3. Artificial nipples should not be given to the baby. There
seems to be some controversy about whether "nipple confusion" exists. Babies
will take whatever method gives them a rapid flow of fluid and may refuse others
that do not. Thus, in the first few days, when the mother is producing only a
little milk (as nature intended), and the baby gets a bottle (as nature
intended?) from which he gets rapid flow, he will tend to prefer the rapid flow
method. You don’t have to be a rocket scientist to figure that one out, though
many health professionals, who are supposed to be helping you, don’t seem to be
able to manage it. Nipple confusion includes not just the baby refusing the
breast, but also the baby not taking the breast as well as he could and thus not
getting milk well and /or the mother getting sore nipples. Just because a baby
will "take both" does not mean that the bottle is not having a negative effect.
Since there are now alternatives available if the baby needs to be supplemented
why use an artificial nipple?
4. No restriction on length or frequency of breastfeedings.
A baby who drinks well will not be on the breast for hours at a time. Thus, if
he is, it is usually because he is not latching on well and not getting the milk
which is available. Get help to fix the baby’s latch, and use compression to get
the baby more milk. This, not a pacifier, not a
bottle, not taking the baby to the nursery, will help.
5. Supplements of water, sugar water, or formula are rarely
needed. Most supplements could be avoided by getting the baby to take
the breast properly and get the milk that is available. If you are being told
you need to supplement without someone having observed you breastfeeding, ask
for someone to help who knows what they are doing. There are rare indications
for supplementation, but usually supplements are suggested for the convenience
of the hospital staff. If supplements are required, they should be given by
lactation aid, not cup, finger feeding, syringe or
bottle. The best supplement is your own colostrum. It can be mixed with sugar
water if you are not able to express much at first. Formula is hardly ever
necessary in the first few days.
6. A proper latch is crucial to success. This is the key to
successful breastfeeding. Unfortunately, too many mothers are being "helped" by
people who don’t know what a proper latch is. If you are being told your two day
old’s latch is good despite your having very sore nipples, be skeptical, and ask
for help from someone who knows.
Before you leave the hospital, you should be shown that your baby is latched
on properly, and that he is actually getting milk from the breast and that you
know how to know he is getting milk from the breast (open—pause—close type of
suck). If you and the baby are leaving hospital not knowing this, get help
quickly.
7. Free formula samples and formula company literature are not
gifts. There is only one purpose for these "gifts" and that is to get
you to use formula. It is very effective, and very unethical, marketing. If you
get any from any health professional, you should be wondering about his/her
knowledge of breastfeeding and his/her commitment to breastfeeding. "But I need
formula because the baby is not getting enough!". Maybe, but, more likely, you
weren’t given good help and the baby is simply not getting your milk well. Get
good help. Formula samples are not help.
Under some circumstances, it may be impossible to start breastfeeding early.
However, most medical reasons (maternal medication, for example) are not true
reasons for stopping or delaying breastfeeding, and you are getting
misinformation. Get good help. Premature babies can start breastfeeding much,
much earlier than they do in many health facilities. In fact, studies are now
quite definite that it is easier for a premature baby to breastfeed than to
bottle feed. Unfortunately, too many health professionals dealing with premature
babies do not seem to be aware of this.
let us be friends with you to enjoy updates on breastfeeding articles and updates.
Dear Members
Add Us as "Friends" to enjoy our daily Readup on Breastfeeding and others Topics Informations.
Thanks
Baby N Me Management
Does Breastfeeding Cause Postpartum Hair Loss?
Postpartum hair loss is a normal – and temporary – postpartum change that is unrelated to breastfeeding. Most women will return to their usual hair growth cycle between 6 and 12 months after birth.
Many new moms notice hair loss – sometimes quite dramatic – around three months postpartum. This is a
normal – and temporary – postpartum change that is unrelated to breastfeeding.
Following is how the hair growth cycle works:
All hair has a growth phase, termed anagen, and a resting phase, telogen. On the scalp, anagen lasts approximately 3 years, while telogen lasts roughly 3 months, although there can be wide variation in these times between individuals. During telogen, the resting hair remains in the follicle until it is pushed out by
growth of a new anagen hair.
From Telogen
Effluvium by Elizabeth CW Hughes, MD
Normally, around 85-95% of your hair is in the growth phase at any point in time, but the hormonal changes
during pregnancy stimulate an increase in the percentage of hairs in the growth phase. As a result, many women enjoy thicker hair during pregnancy, as more hairs than normal are growing and fewer than normal are resting/shedding.
With the birth of your baby (and the hormonal changes that accompany birth), a larger number of hairs than normal enter the resting phase. Since the resting phase is followed by hair shedding (and regrowth), new mothers will experience greater than normal hair loss once the resting phase ends.
Postpartum hair loss commonly starts at around three months after birth. The amount of time between childbirth and the onset of shedding corresponds to the length of the resting phase of hair growth (between 1 and 6 months, with an average of three months). The hair loss can seem more extreme if your hair grew much more than normal during pegnancy, or if you have long hair. Most women will return to their usual hair growth cycle within six months, or between 6 and 12 months after birth.
If you feel that your hair loss is greater than the norm, or if things are not back to normal by the time your baby is 12 months old, then see your doctor. Excessive hair loss can be caused by common and easy-to-remedy postpartum conditions such as hypothyroidism (low thyroid hormone) or iron-deficiency anemia.
What can you do while you wait for your hair to return to its normal growth cycle?
■Get a good haircut.
Some moms choose this time to get a shorter haircut or one that requires less care.
■Experiment with different hairstyles.
■A good quality shampoo and conditioner may help.
■Try different styling products, such as mousses or texturizers that “bulk up” the appearance of your hair.
■Avoid using a brush or comb that pulls or stresses the hair.
Many new moms notice hair loss – sometimes quite dramatic – around three months postpartum. This is a
normal – and temporary – postpartum change that is unrelated to breastfeeding.
Following is how the hair growth cycle works:
All hair has a growth phase, termed anagen, and a resting phase, telogen. On the scalp, anagen lasts approximately 3 years, while telogen lasts roughly 3 months, although there can be wide variation in these times between individuals. During telogen, the resting hair remains in the follicle until it is pushed out by
growth of a new anagen hair.
From Telogen
Effluvium by Elizabeth CW Hughes, MD
Normally, around 85-95% of your hair is in the growth phase at any point in time, but the hormonal changes
during pregnancy stimulate an increase in the percentage of hairs in the growth phase. As a result, many women enjoy thicker hair during pregnancy, as more hairs than normal are growing and fewer than normal are resting/shedding.
With the birth of your baby (and the hormonal changes that accompany birth), a larger number of hairs than normal enter the resting phase. Since the resting phase is followed by hair shedding (and regrowth), new mothers will experience greater than normal hair loss once the resting phase ends.
Postpartum hair loss commonly starts at around three months after birth. The amount of time between childbirth and the onset of shedding corresponds to the length of the resting phase of hair growth (between 1 and 6 months, with an average of three months). The hair loss can seem more extreme if your hair grew much more than normal during pegnancy, or if you have long hair. Most women will return to their usual hair growth cycle within six months, or between 6 and 12 months after birth.
If you feel that your hair loss is greater than the norm, or if things are not back to normal by the time your baby is 12 months old, then see your doctor. Excessive hair loss can be caused by common and easy-to-remedy postpartum conditions such as hypothyroidism (low thyroid hormone) or iron-deficiency anemia.
What can you do while you wait for your hair to return to its normal growth cycle?
■Get a good haircut.
Some moms choose this time to get a shorter haircut or one that requires less care.
■Experiment with different hairstyles.
■A good quality shampoo and conditioner may help.
■Try different styling products, such as mousses or texturizers that “bulk up” the appearance of your hair.
■Avoid using a brush or comb that pulls or stresses the hair.
A Testimonial to share from a happy mummy who believe our Sacred Tea that has help her motherhood.
I would like to thank you for bringing in Sacred Tea. It does wonders for boosting my milk supply. For the record, I started talking Sacred Tea when I had my big boy, my milk supply was decreasing drastically on the 3rd month as I was falling sick all the time due to poor confinement, to add on during my son 2nd week of life, I almost lost him to GBS (late onset), he was hospitalised for 2 weeks with countless drips, injections, blood test daily and not to forget lumber puncture too. As a mother, I felt helpless and frustrated for not being able to alleviate the situation nor can I give him sufficient milk due to escalated stress.
Things start to take a good turn when I chance upon Sacred Tea over the web and I thought to myself that things couldn’t get any worse than this and decided to give it a try. My milk supply started to gradually increase a little the next day from 70 – 90 ml, I followed the instructions on a healthy diet, latch/express every 3 hourly and drink plenty of fluids eventually I could produce more and more milk, 150 – 200 ml every 3 hours.
Now with my 2nd child, I drank Sacred Tea immediately after delivery my baby girl, not only I have more colostrums compared to my 1st boy, my milk kicks in on the 3rd days. (For C-section delivery, my gynae said this is very fast.) By the 8th days, I had 2.5 litres of extra frozen EBM, my daughter is being breastfeed exclusively, and in fact I have so much that I am also feeding my older boy with my EBM.
FYI, my hubby bought 2 tins of formula assuming I would not have sufficient milk like last time.
Hee... Hee...
Thanks you Sacred Tea, You made me a Happy Mummy with Happy Babies.
Yours Sincerely
Diany Tai
I would like to thank you for bringing in Sacred Tea. It does wonders for boosting my milk supply. For the record, I started talking Sacred Tea when I had my big boy, my milk supply was decreasing drastically on the 3rd month as I was falling sick all the time due to poor confinement, to add on during my son 2nd week of life, I almost lost him to GBS (late onset), he was hospitalised for 2 weeks with countless drips, injections, blood test daily and not to forget lumber puncture too. As a mother, I felt helpless and frustrated for not being able to alleviate the situation nor can I give him sufficient milk due to escalated stress.
Things start to take a good turn when I chance upon Sacred Tea over the web and I thought to myself that things couldn’t get any worse than this and decided to give it a try. My milk supply started to gradually increase a little the next day from 70 – 90 ml, I followed the instructions on a healthy diet, latch/express every 3 hourly and drink plenty of fluids eventually I could produce more and more milk, 150 – 200 ml every 3 hours.
Now with my 2nd child, I drank Sacred Tea immediately after delivery my baby girl, not only I have more colostrums compared to my 1st boy, my milk kicks in on the 3rd days. (For C-section delivery, my gynae said this is very fast.) By the 8th days, I had 2.5 litres of extra frozen EBM, my daughter is being breastfeed exclusively, and in fact I have so much that I am also feeding my older boy with my EBM.
FYI, my hubby bought 2 tins of formula assuming I would not have sufficient milk like last time.
Hee... Hee...
Thanks you Sacred Tea, You made me a Happy Mummy with Happy Babies.
Yours Sincerely
Diany Tai